Newsletters
- Home
- Publications
- Newsletter Archive
- Newsletter
November/December 2002
Inside This Issue:
- The Impacts of Federal Legislation on Rural Home Health Care
- Chairman's Message
- Helpful Hints on Getting that Grant
- Center-Sponsored Health Initiative Receives $387,000 Federal Funding
- Comments Roll In During Rural Forums
- Did you know . . .
- Update: Census 2000
- Rural Farm and Non-Farm Populations
- Just the Facts: Property Taxes
The Impacts of Federal Legislation on Rural Home Health Care
Health care delivery to rural areas is a challenge. From the family doctor to the acute care hospital, health care providers and institutions in rural areas are under pressure to meet the needs of the state's population - a population that continues to grow older.
An integral component of the rural health care delivery system is Medicare-funded home health agencies. Home health agencies are home care providers that offer therapeutic and skilled and supportive post-acute care nursing services for homebound patients and provide clinical services for chronic conditions, such as diabetes. The importance of Medicare home health services has grown as the nation attempts to shift health care away from expensive modes of delivery, such as hospital and long-term care, into less costly service delivery methods like home health.
Federal legislation, specifically the Balanced Budget Act of 1997, has the potential to compromise both the financial viability of rural home health agencies and the level of service that they provide to their patients. The legislation cut the total amount of Medicare reimbursements to home health agencies and forced them to assume more financial risk by changing the reimbursement method from one based on the agency's cost to a fixed-rate schedule. The smaller the agency, the greater the potential risk. This is why the change in reimbursement methods is of great importance to rural residents of the commonwealth.
To learn how the Medicare home health provisions of the Balanced Budget Act of 1997 are affecting rural home health agencies and the services they provide to rural patients, the Center for Rural Pennsylvania sponsored a one-year grant project, conducted by Lisa A. Davis and Myron R. Schwartz of the Pennsylvania Office of Rural Health at Penn State University, and by Dr. Joel Leon, Joan K. Davitt, and Jonas Marainen, of the Edward and Esther Polisher Research Institute. The results of that project, entitled The Effect of New Medicare Reimbursement Methodologies on Rural Home Health Agencies and Their Beneficiaries, are now available.
Payment methods set in motion
The Medicare home health provisions of the Balanced Budget Act
of 1997 set into motion two sequential payment methods. The first,
an Interim Payment System (IPS), operating from 1998 to 2000,
was implemented to immediately control spending under the then
existing cost-based system, a system that paid agencies based
on the actual cost of providing each visit. Under IPS, total national
expenditures for home health care declined by 44 percent from
16.2 billion dollars in 1997 to 9 billion dollars in 2000. The
second payment method, the Prospective Payment System (PPS), set
into place a case-mix system that would permanently build efficiency
incentives into the home health payment structure and pay agencies
on a prospective rather than a cost reimbursement method. The
PPS transfers financial risks to providers, and in so doing, has
the potential to result in the provision of fewer services and
the avoidance of high cost patients. The PPS went into effect
in late 2000 and evaluations of its impact are not widespread.
Research goals
The goals of the research project sponsored by the Center were
to assess the financial effects of the new reimbursement methodologies
on rural home health agencies and analyze patterns in these effects;
assess the effects of the new reimbursement methodologies on beneficiaries
of rural home health agencies and analyze patterns in these effects;
document levels of home health service and utilization across
the commonwealth and analyze changes in these levels over time;
and formulate policy recommendations.
The researchers used and integrated five major data sources to achieve the results of the research. The data sources included:
-
a survey of administrators in all rural home health agencies in Pennsylvania;
-
Medicare agency cost reports for fiscal years 1996 and 1999;
-
individual claims data for fiscal years 1998 and 2000;
-
1990 and 2000 Decennial Census data and compatible geographic information system (GIS) files; and
-
interview data with home health experts (key informants).
Key findings offered
From the study, the researchers identified seven key findings.
1. There are fewer home health agencies serving the commonwealth and they operate fewer branch offices than prior to the implementation of the new reimbursement methodologies.
2. There are fewer users of Medicare home health services than before the implementation of the new reimbursement methodologies. This pattern is true for most of the commonwealth.
3. There is variance in the rate of use of Medicare home health services across the commonwealth. Rural areas include areas of both high and low use. High use areas are disproportionately represented in the western half of the commonwealth and low use areas in the eastern half.
4. Medicare home health agencies are operating under more financially challenging circumstances than before the implementation of the new reimbursement methodologies. The agencies' total revenues are significantly lower, and the agencies must manage more financial risk in treating certain high cost patients.
5. Medicare agencies operate under more administratively challenging conditions than before the implementation of the new reimbursement methodologies. These conditions include implementation of the Outcome and Assessment Information Set (OASIS) assessment procedures, managing financial risk, and managing fewer visits per patient to accommodate the episode-based payments of PPS.
6. Certain high cost patients may find it more difficult to obtain traditional Medicare home health services than before the implementation of the new reimbursement methodologies, and other patients more frequently may have to confront the necessities of their Medicare home health provider spending less time on care.
7. Because of more restricted use and service levels for traditional Medicare home health than before the implementation of the new reimbursement methodologies, users are being referred to other publicly supported services in the commonwealth.
Specific activities to pursue
The results of the research suggested some specific activities
that may benefit the commonwealth. First, service delivery to
patients has changed significantly since the implementation of
the new reimbursement methodologies. However, the details associated
with these changes, especially for high cost patients, have yet
to be documented. The researchers suggest that commonwealth agencies
with an interest in home health, such as the Departments of Health,
Public Welfare, and Aging, fully document the level and variance
in service provision.
Second, the regional variation in rates for Medicare home health use is quite striking. Commonwealth agencies with a vested interest in home health need to make sure that regional access inequalities do not exist in the commonwealth.
Third, the administrative burden under the new reimbursement methodologies is quite demanding for small rural agencies. The commonwealth should consider offering technical assistance to these agencies directly or through associations.
Next, since some patients are being diverted from Medicare home health to other commonwealth services, the commonwealth should consider increasing support for rural Area Agencies on Aging and Medical Assistance to assist those patients who are unable to get adequate (or any) home health care services through Medicare.
Lastly, rural home health agencies receive a 10 percent add-on to their reimbursements for Medicare. The add-on was about to expire when the research was being completed. The researchers suggested that to avoid further taxing commonwealth resources, state legislators should approach the Pennsylvania Congressional delegation and ask that it seek a continuance of the add-on. (Editor's note: In May, the Pennsylvania General Assembly passed House Resolution 576, which urged Congress to extend the 10 percent rural add-on. Congress provided for a continuance of the add-on until spring 2003.)
Want more info?
For a copy of the report, The Effect of New Medicare Reimbursement
Methodologies on Rural Home Health Agencies and Their Beneficiaries,
call the Center for Rural Pennsylvania at (717) 787-9555 or email info@ruralpa.org.
Chairman's Message
According to the National Center for Health Statistics, in 2000, the average life expectancy for all Americans was 76.9 years of age; more specifically, 74.1 for males and 79.5 for females. That's wonderful news for our nation and testament to the advances in nutrition, medicine, and health care.
As we focus on helping our population to live longer and to continue leading active lives, it's not hard to understand why health care services and delivery have become some of the most pressing issues facing our nation and our state.
For rural Pennsylvanians, the adequacy and availability of health care services and delivery are major concerns. To better understand the questions surrounding the issues, the Center for Rural Pennsylvania has focused much of its research on a variety of health care topics over the years.
This past year, researchers from Penn State University and the Edward and Esther Polisher Research Institute studied the Medicare home health provisions of the Balanced Budget Act of 1997.
Medicare-funded home health agencies are an integral component of the rural health care delivery system, and as the nation attempts to shift health care away from more expensive forms of delivery, such as hospital and long-term care, into less costly service delivery methods like home health, the importance of Medicare home health services has grown.
The results of the research provide important information and recommendations for health care providers and policy makers at the state and national levels. For more on the research, turn to the feature article on page 1.
Another health-care-related initiative sponsored by the Center for Rural Pennsylvania is also reaping positive results. The pilot project, which was conducted by the Penn State College of Medicine at the Milton S. Hershey Medical Center, was instrumental in demonstrating the viability of a technology approach to education. The project has received additional funding from the federal government to continue and expand the program over the next three years. See the related article on page 4 for more information.
Also on page 4 are some helpful hints on developing a successful grant application. If you or your organization have ever applied for a grant, you know that the process can sometimes be confusing or even frustrating. The article on getting that grant will hopefully take some of the guesswork out of grant writing, and more importantly, help to secure those funds.
As we study the comments received from the Rural Definition Forums that were held throughout the state in October, we are reminded of the diversity of our rural state. The rural forums were a great opportunity for the Center's Board members to learn your thoughts on defining "rural" for Pennsylvania and we will depend heavily on your comments as we work to develop that designation. Thank you again for your participation in the forums and your comments.
We look forward to sharing the results of those meetings with you in the months ahead.
Representative Sheila Miller
Helpful Hints on Getting that Grant
Have a great idea for a community project but no dollars to make it happen? Many state, federal, and non-profit organizations have grant funds that can help get your project off the ground. To give you a better idea on what it takes to write a grant and get your hands on that funding, the Center for Rural Pennsylvania's Program Manager for Grants offers the following tips to get you started.
Sounds like a plan
Translate your great idea into a plan of action. Funding agencies
like to know, specifically, how the grant funds will be used and
how the funds will make a difference. Make sure that your project
focuses on a real need for your community, organization or topic
area. For instance, don't just ask for money for computers. Describe
why you need the computers and how a community problem will be
affected. For example, explain how a pilot after-school computer
program for middle school youth is helping to eliminate the vandalism
problem in your community.
Convince the funding source that you have a plan that can solve the problem and that your plan is appropriate for your community. Funding agencies want to see that you are addressing a documented need that will result in measurable positive impact.
Research your funding source
Since there are many kinds of funding agencies that might be a
source of funds for your project, do some legwork. A good place
to start is the Center for Rural Pennsylvania's
Rural Access Guide, which is available online at www.ruralpa.org and lists general information and contacts for state, federal
and non-profit grants, loans and technical assistance. Another
great starting point is your local library, which has information
and publications on other funding sources.
Make sure that your organization is eligible for the grant you are interested in and that the funding source makes grants in the amount you are after. If you are not eligible, consider partnering with an organization that is.
Fill in the blanks
Don't assume that the funding source is familiar with your community
or with jargon that may be specific to your topic area. Everyone
in town may know that the drinking water is bad, but a funder
sitting in Harrisburg or Washington may not. Paint the picture
with facts to make your case. Provide quantitative and qualitative
evidence of the need as support for your proposed solution. The
Center for Rural Pennsylvania can provide you with demographic
information about your community that will help you make your
case. Check our website or call for specifics.
Show it is a "can-do" project
No one wants to pay for something that will not have any results.
Provide as much evidence as possible that your project will result
in measurable positive outcomes. How will you document that a
grant for extended hours at the community library has been good
for the community? Include evaluation in your work plan.
Follow up
Finally, if you are not successful in winning the grant, contact
the funding source and ask for feedback. This may help you target
your application to successfully secure that grant in the next
round.
Center-Sponsored Health Initiative Receives $387,000 Federal Funding
A pilot project to encourage the retention of rural physicians, funded by a $15,000 Center for Rural Pennsylvania initiative in 2001 and administered by Penn State University's Center for Primary Care at the Milton S. Hershey Medical Center, has met with considerable success. The project involved rural physician practice sites where third-year medical students were assigned in a Preceptor Training Program. The Center for Primary Care created a special website for access by the rural physician preceptors and medical students. The pilot project was instrumental in demonstrating the viability of a technology approach to education, retaining rural preceptors, and helping to improve patient care. The results from the pilot project resulted in the funding of a three-year, $387,000 faculty development grant from the federal Health Resources Service Administration to continue and expand the program to include 280 physician preceptors across Pennsylvania.
For more information about the development grant, contact Dr. John George, Director of Predoctoral Education, Penn State College of Medicine, Penn State Milton S. Hershey Medical Center, Family and Community Medicine, H154, 500 University Drive, PO Box 850, Hershey, PA 17033-0850, telephone (717) 531-8736.
Comments Roll In During Rural Forums
 Representative Sheila Miller welcomes participants to the Harrisburg Rural Definition Forum. |
Representative Miller welcomed more than 70 attendees to the forum, which was held at the Hospital and Health-system Association of Pennsylvania.
The forums, which were also held in Franklin, Lock Haven, Greensburg, Towanda and West Chester, were attended by municipal officials, planners, hospital administrators, grant writers, and other data users from around the commonwealth.
The input received from the forum attendees will help the Center's Board of Directors to determine the best way to designate counties and other entities as rural or urban according to Census 2000 data.
 Lisa Davis (standing at podium), executive director of the Pennsylvania Office of Rural Health, answers questions related to her presentation on rural health from the 2000 Census. Amy Jonas of the Center for Rural Pennsylvania is standing at left. |
 Jonathan Johnson of the Center for Rural Pennsylvania offers discussion points for the forum. |
Senator Mary Jo White, Center Board treasurer, hosted the October
10 forum in Franklin and Representative Mike Hanna and Lock Haven
University President Craig Willis, Center Board members, hosted
the October 11 session at Lock Haven.
To learn more about the information presented at the forums, visit
the Center for Rural Pennsylvania's website at www.ruralpa.org or call the Center at (717) 787-9555.
Did you know . . .
-
According to the U.S. Census Bureau, rural Pennsylvania is geographically bigger than 15 states and 94 countries.
-
Census data shows that between 1990 and 2000, the number of people born between 1946 and 1964 (Baby Boomers) in rural Pennsylvania increased nearly 7 percent. In urban areas, there was a 2 percent decline in Baby Boomers.
-
According to the 2000 Census, there are more people in rural Pennsylvania under 12 years old than there are People 65 years old and older.
-
According to the U.S. Patent and Trademark Office, more than 2,500 patents were issued to rural Pennsylvanians between 1990 and 1999. Rural Pennsylvanians secured more patents than those living in 14 other states.
Update: Census 2000
SF4 Detailed Socio-Economic Data by All Races To Be Released
It's finally here. The Summary File 3 (SF3), which contains the nitty-gritty socio-economic data from the 2000 Census, was released for Pennsylvania on September 25. Now we can more closely examine our communities for such items as poverty, disability status, and housing values. This detail will be available for any census geography from the nation down to the Census tract.
Most importantly for rural data users is the availability of the community level data on rural and urban populations. This includes breakdowns of populations in urbanized areas, urban clusters, rural farm, and rural non-farm.
While there are some breakdowns in SF3 in terms of race, the next file, SF4, will cross all SF3 variables by detailed race categories and by ancestry. This upcoming file will allow data users to look at characteristics such as housing values for Chinese homeowners or language spoken at home by those of German ancestry. But we still have a bit of a wait since SF4 is due to be released a few states at a time from April through September 2003.
For more Census 2000 information, visit the U.S. Census Bureau's website at www.census.gov or call the Center for Rural Pennsylvania at (717) 787-9555.
Note: Be careful when comparing Census 2000 SF3 data with Census 1990 STF3 data since some questions were asked differently during the two censuses and therefore may not be perfectly comparable.
Rural Farm and Non-Farm Populations
As the Center for Rural Pennsylvania wrestles with the formula for a working definition of rural within the commonwealth, it may be a good time to look at how the rural population has changed according to the U.S. Census Bureau. Census 2000 data show that Pennsylvania's 2.8 million rural residents account for 23 percent of the state's total population.
The Census divides the rural population into rural farm and rural
non-farm residents.
The rural farm population consists of people living in farm residences.
A household is a farm residence if: (1) the housing unit is located
on a property of one acre or more, and (2) at least $1,000 worth
of agricultural products were sold from the property in 1999.
People, such as farm workers, who reside in multi-unit buildings
or group quarters on a farm property are excluded from the farm
population.
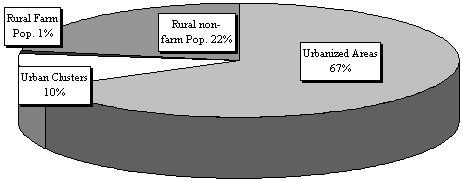
Less than 1 percent of Pennsylvania's population was classified as rural farm, while about 22 percent was classified as rural non-farm.
The rural population in Pennsylvania grew in each Decennial Census since 1970 until the definition change of 2000, at which time the numbers dropped dramatically.
The rural farm population, however, declined with each Census, regardless of definition, showing that fewer and fewer people are living in households on farms in the commonwealth. Over the same period, the urban population continued to decrease from 1970 on and then took a huge leap in 2000 with the change in definition.
Rural and Urban Pennsylvania Population
Shares, 2000
Just the Facts: Property Taxes
Most everyone loves to hate real estate property taxes. But no matter what your feelings are for property taxes, the fact is that for rural Pennsylvania's 1,500 local governments, counties, and school districts, these taxes are a critical source of revenue. According to data from the Center for Local Government Services and the Pennsylvania Department of Education, in 2000-2001, rural Pennsylvanians collectively paid nearly $1.5 billion in property taxes, or $569 per person to support local services, infrastructure, and education. In urban areas, the total real estate tax bill came to almost $8.4 billion, or $864 per person.
In rural areas, nearly 73 cents out of each dollar collected in property taxes, or $1.1 billion, went to help finance school districts. This amount, however, only provides about 33 percent of total revenues to the average rural school district. For urban schools, these taxes provide nearly 47 percent of school district revenues. The difference is partially due to differences in the amount of state funding received by rural and urban districts. The state provides monies to school districts based on need, enrollment, and other factors. During the 2000-2001 school year, rural districts received 49 percent of their total revenues from the state, while urban districts received 34 percent. Over the last 10 years, the importance of property tax receipts as a percentage of total district revenues has remained fairly constant for both rural and urban schools.
As total school district revenues have increased, so have property tax revenues. Adjusted for inflation, the property tax receipts among rural schools have increased 30 percent between 1991 and 2001. This rate is nearly identical to the urban rate. The increase in property tax receipts does not necessarily mean that land and homeowner tax rates have increased. Among rural schools, the increase in property tax receipts is more a result of increasing property values rather than increasing tax millage.
Between 1990 and 2000, the market value of real taxable property increased 30 percent in rural areas. This increase means that each mill of tax generated more revenue. Evidence of this increased value can be seen in the ratio of real estate taxes to market values. In both 1991 and 2000, rural school districts collected 1.4 percent of the market value of real estate.
A comparison of school tax payments by rural and urban residents shows that in 2001, using equalized mills, which is the total taxes collected divided by total market values, rural areas had a millage rate of 19.0 while urban areas had a slightly higher rate of 20.8 mills.
If all of this talk about taxes is getting you down, consider
this: according to the U.S. Census Bureau, Pennsylvania ranked
26th in local government property taxes per capita, in 1998, with
each resident paying $740. New Jersey, New Hampshire, and Connecticut
residents each paid more than $1,470 in local government property
taxes per capita. Kentucky, New Mexico, and Alabama residents
each paid less than $300 per capita.
